
Preventive Care for Birmingham Women
A few generations ago, cervical cancer took the lives of more women than any other cancer. Today, it is a largely preventable disease. Beginning in the 1940s, the Pap test became available to women. A swab is used to collect cells from the cervix. The sample is then examined to look for abnormal cells, either cancer or pre-cancerous cells.
By the 1990s, research determined that human papilloma virus (HPV) causes cervical cancer. This discovery opened the door to new preventive opportunities. The HPV vaccine, given to preteens and young adults, can provide strong protection against cervical cancer. We now have a test for the presence of the HPV virus from a swab of the cervix. It can be performed alone or at the same time as a Pap test. The HPV test tries to find the virus that could cause cancer or pre-cancer. It does not look at whether cervical cells are normal or abnormal.
Why then do 12,000 women in the U.S. still develop cervical cancer each year? First, for a number of reasons, many women do not get regular preventive healthcare services. Second, the number of young women getting the complete series of HPV vaccines is much lower than we would like—in Alabama only about 58%. Finally, neither the vaccine nor the Pap and HPV tests provide 100% protection.
From their first Gyn exam, women have traditionally expected a Pap test every year. Only recently, some health-policy makers have changed their recommendations. The United States Preventive Services Task Force (USPSTF) and other organizations now recommend the following screening schedule:
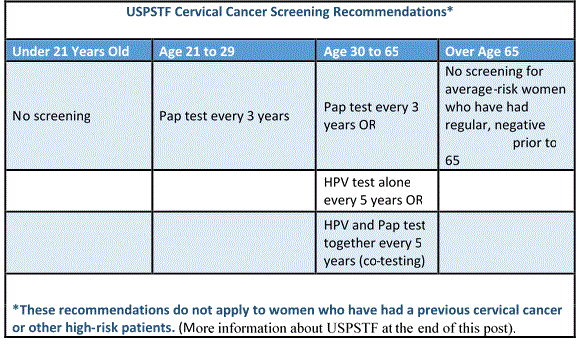
The new recommendation attempts to balance the benefit of cervical cancer screening against the need for additional examinations or treatment—and the resulting anxiety—when no cancer was actually present or was likely to develop. This strategy does not claim to provide 100% protection, but rather a reasonable balance between protection and the harms described above. Many doctors feel that Pap tests should be performed more frequently than this schedule recommends.
Usually we perform a Pap test at your annual exam regardless of the interval since your last Pap test. We do this because:
- A single Pap test can fail to identify pre-cancerous cells when they are present (a false-negative result). With a series of regular normal Pap tests, the chance that more than one of the most recent tests are false-negatives becomes much lower.
- The HPV test alone—without the Pap test–is now approved for screening; however, like the Pap test, it too has some false-negative results.
- Co-testing using the HPV test AND Pap test every 5 years for women age 30 thru 65 reduces the risk of a false-negative result to a very low percent, but not zero. The time interval until you are screened again is longest with this method.
- We cannot know which patient will lapse in seeing her physician for regular preventive care. If a woman misses one or more annual exams, that extends the length of time since her last normal Pap test—even longer if her last test happened to give a false negative result.
- We offer cervical cancer screening to our patients over 65 because the rate of new cervical cancer cases for a woman age 65 to 69 is the same as for a woman in her early thirties. Risk decreases only modestly from 65 to the end of a woman’s life.
- Finally, when your physician is performing your annual pelvic exam, the extra screening adds little or no time or discomfort.
A woman who follows the current USPSTF guidelines has a very low cancer risk. More frequent testing will further reduce cancer risk. But it also increases the chance of an abnormal result when no cancer or pre-cancer exists (a false-positive result).
Remember that the Pap is just a test, NOT an exam. With or without a Pap test, you should still have a well-woman exam every year. During the GYN exam, your doctor evaluates the entire reproductive tract—checking for pelvic masses, possible cancers on the external genital skin or vagina, and performs a clinical breast exam. If you’ve had a hysterectomy, your doctor will advise you about whether to continue having Pap tests. The annual GYN exam also provides a chance for a more comprehensive wellness assessment. We can update your family risk history, recommend immunizations, check routine lab studies (like cholesterol, glucose, blood count, urinalysis), provide birth control options and support with weight management, smoking cessation, etc.
We welcome your questions about cervical cancer screening. Please inform us at the time of your exam if you prefer the less frequent screening described in the USPSTF August 2018 statement.
*The USPSTF is an organization set up to create guidelines for the use of preventive healthcare services. Preventive services are any tests or treatments that attempt to find or prevent illness before an individual shows any signs or symptoms of that illness. The USPSTF’s recommendations can affect your access to preventive services. Under the Affordable Care Act your private health insurance is required to pay (without a co-pay from you) for services that receive an A or B level USPSTF recommendation. Task Force members are appointed by an agency within the U.S. Department of Health and Human Services.