 Surprising Facts:
Surprising Facts:
Over 40% of women’s health providers choose the Intrauterine Device (IUD) for themselves according to one study. However, The American College of Obstetricians and Gynecologists reports that only about 12% of American women overall are choosing an IUD or other long-acting reversible contraception methods (LARC). These gynecologists and other providers help their patients learn about the advantages they enjoy themselves. Long-acting reversible contraceptive (LARC) methods like the intrauterine device (IUD) and arm implant (Nexplanon) are very reliable types of birth control that provide years of protection against pregnancy with a single device.
Why Do So Many Women’s Doctors Choose LARC?
These birth control methods are the gold standard for reliability and convenience while also being reversible. They work for between 3 and 10 years depending on the device chosen, and they are 99% effective at preventing pregnancy! You don’t have to remember to do something every day. Your partner usually can’t tell you have the device in place.
The IUD and Nexplanon are completely reversible methods. If you decide you want to get pregnant, you can have either one removed, and fertility can return soon afterward. Some women have health risk factors that exclude them from taking the birth control pill with estrogen. LARCs do not contain estrogen, so more women are eligible to have them. The American Academy of Pediatrics considers LARC a safe option for adolescents as well.
How Do These Devices Work?
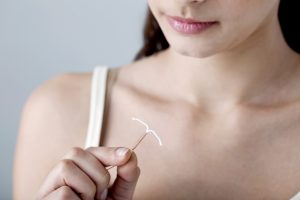
Intrauterine Device (IUD):
IUDs are small, plastic T shaped devices that are placed into the uterine cavity. There are two types: non-hormonal and hormonal. Both work by preventing fertilization of the egg by sperm.
The copper IUD (Paragard) is non-hormonal. It works because copper interferes with sperm’s ability to move. It also thickens cervical mucus to make it harder for sperm to get to the egg. It is good for 10 years. It does not prevent ovulation, and you still have a monthly period. It may make your period heavier, especially in the first 6 months of use.
There are several brands of hormonal IUDs that have different lengths of use from 3 to 7 years. The brand names include Mirena, Skyla, Liletta, and Kyleena. They each contain a progesterone hormone called levonorgestrel (LNG). The hormone, which is slowly released, helps thicken cervical mucus and thin the lining of the uterus. Over a few months, periods usually become shorter, lighter, or may stop altogether. The progestin effect makes hormonal IUDs a good birth control choice for women who experience painful periods or heavy bleeding. The Mirena IUD is FDA approved to treat heavy bleeding in addition to being a contraceptive device. In one study, 90% of women who got the Mirena showed a decrease in amount of menstrual bleeding after 6 months.
Arm Implant:
The Nexplanon device is a small rod that is inserted in the upper arm just under the skin above the elbow. It releases a small amount of progesterone hormone every day that stops your ovaries from ovulating (releasing an egg). This hormone also thins the lining of the uterus over time. It is hard to predict how your periods will be on Nexplanon. Some people have irregular bleeding, light periods, spotting, no periods. Others have their normal period.
What are the Disadvantages of IUDs and Nexplanon?
LARC methods do not protect against STIs like condoms do. They may disrupt or change your period or cause irregular bleeding. Some women using LARC methods do not have a period. This is more common with the hormonal IUD. Copper IUDs can increase heavy periods and painful period cramps. Insertion can be uncomfortable. Your doctor can place numbing medicine to help with the discomfort. The IUD can get in the wrong place, called malposition, or go through the wall of the uterus, called perforation. Sometimes surgery is required to remove it if this occurs. Perforation is uncommon. If you do get pregnant while an IUD is in place, there is an increased risk the pregnancy may not be in your uterus (ectopic pregnancy). The IUD can also fall out. IUDs can’t be placed if you have a sexually transmitted infection.
The Nexplanon implant can move in your arm away from the spot it was placed. If irregular spotting or bleeding occurs, this may be inconvenient. Some women also report mood swings or depression, weight gain, acne, and headaches when using the Nexplanon.
Not everyone experiences these side effects. Keep in mind that, compared to other types of birth control like pills, the patch, the vaginal ring, and condoms, LARCs are 20x more effective over several years of use.
What to Expect at Your Office Visit for LARC Insertion
For the IUD, a pelvic exam is performed, where a speculum is inserted to view the cervix. The cervix is cleaned with an antiseptic solution. Your doctor measures the uterus length before inserting the device. After the IUD is inserted, the strings are trimmed, and the speculum is removed. The process of inserting an IUD usually takes less than 10 minutes. When you decide you want the device removed or it is about to expire, a pelvic exam is again performed. As long as the strings are visible at the cervix, they are grasped, and the device is removed.
For the arm implant, your gynecologist will measure on your upper arm to find the right place to insert the device. The arm is then cleaned with an antiseptic solution. Numbing medicine is injected under your skin. Once the numbing medicine takes effect, the Nexplanon device can be inserted under your skin. After insertion, your doctor will ask you to feel where the device is in your arm. A pressure bandage will be placed at the insertion site that will need to stay on for about 24 hours to help the site heal.
When you decide you want the Nexplanon removed, your doctor will feel the device in your arm. They will clean off the area and insert numbing medicine. Once the area is numb, they will make a small incision in your arm to be able to use a grasper to locate and remove the Nexplanon. Sometimes there is scar tissue around the device that may make it take longer to remove. If your doctor is not able feel in your arm, you may need an x-ray or ultrasound to locate it before removal.
No method of birth control is a good choice for every woman. Your gynecologist will help you to consider risks and benefits and determine the best option for you individually. Call our office to set up an appointment to discuss options with your doctor. You can read more about who is a good candidate for IUD use and some of its risks in the patient FAQ “Long-Acting Reversible Contraception (LARC): IUD and Implant” from the American Congress of Obstetricians and Gynecologists.
Sources:
www.contraceptionjournal.org/article/S0010-7824%2815%2900072-4/pdf
American College of Obstetricians and Gynecologists