In my practice as a Birmingham gynecologist, I must occasionally convey to a woman that she is facing ovarian cancer. Around 20,000 American women are newly diagnosed each year. When ovarian cancer is discovered at an early stage, the chance of surviving the disease is good. Unfortunately, ovarian cancer has no specific symptoms in its early stage, and no accurate screening tests exist to help physicians diagnose it early. Advanced ovarian cancer is very serious and very difficult to treat. Among American women, it causes more deaths than any other gynecologic cancer. But now women’s physicians are discussing an important new prevention strategy.
We now believe that most cases of advanced ovarian cancer arise—not from the ovary itself—but rather, from the fallopian tube. This new information may influence a shift in the mindset of physicians and women as they make certain healthcare decisions.
What’s New
In November 2013, the Society of Gynecologic Oncology (SGO)—gynecologists specializing in women’s cancer treatment— released a statement to women’s physicians. In short, the SGO announced that removal of the fallopian tubes may be an “appropriate and feasible” strategy for reducing ovarian cancer risk. The statement will certainly impact how physicians counsel their patients. And even the great majority of women whose ovarian cancer risk is average may begin to consider this new information in the decisions they regularly make about their reproductive health. For example:
In the U.S., around 600,000 women undergo a hysterectomy each year (removing the uterus or womb). In many younger women, the ovaries are left in place because they are still active, producing hormones. Now these women need to know that removing the fallopian tubes (leaving the ovaries) at the time of their hysterectomy may reduce their ovarian cancer risk. The tubes carry a woman’s egg from the ovary to the uterus. They have no function after childbearing is complete.
Roughly one in four women chooses tubal ligation surgery to prevent future pregnancies. In light of the SGO statement, these women can discuss with their physicians the option to remove the tubes entirely, rather than just cutting or interrupting a part of each tube. Furthermore, women and their partners often weigh the options of vasectomy (male sterilization) vs. tubal ligation. The possibility that removing the fallopian tube could reduce a woman’s ovarian cancer risk should be added to the discussion.
Although the lifetime risk of ovarian/fallopian tube cancer is less than 2%, an individual woman in that group faces a very difficult and uncertain future. A large amount of data will be needed to know with certainty whether removing the fallopian tubes reduces the likelihood of dying from these cancers. In the meantime, physicians must advise their patients, as they would advise a close family member, based on their clinical judgment about potential benefits and minimal risks.
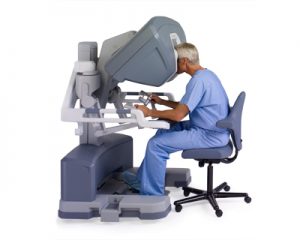
Women need to become informed about this option, especially in situations where removing the tubes is possible without “extra” surgery. A surgeon skilled in minimally-invasive techniques (robotic and laparoscopic surgery) can, in most instances, remove the fallopian tubes fairly easily through the same very tiny incisions used for the hysterectomy or tubal ligation.
Insight into how ovarian cancer develops has also expanded options for women who carry a defective BRCA gene. Because these women have a very high genetic risk for the disease, we recommend complete removal of the ovaries and fallopian tubes after they have completed childbearing plans. If this surgery is undertaken before a woman’s ovaries have stopped functioning (menopause), she will enter an early menopause. Younger women face a difficult decision. A woman who is years away from natural menopause may choose to postpone the surgery in order to delay health and lifestyle effects that menopause may produce. The delay will give her a higher cancer risk during that period of time. For these women, removing only the fallopian tubes may offer them some protection until they are ready to consider removal of the ovaries.
Removing the fallopian tubes for cancer-risk reduction at the time of another gynecologic surgery is an important new concept in women’s healthcare. I am hopeful that, as women and their physicians begin to choose this option, data will show that many lives have been saved.