Slightly more than 1 in 3 American women will develop cancer in her lifetime. Cancer is the second leading cause of death for women (after heart disease). True, it usually strikes during or after middle-age. About 77% of cancers are discovered in people 55 or older. But even if, as you are reading this, “middle-age” seems a long way off; consider that your ability to influence many cancer risk factors begins much earlier in life. Some of the facts I mention here are well-known, but you’ll also find some new insights if you read on.
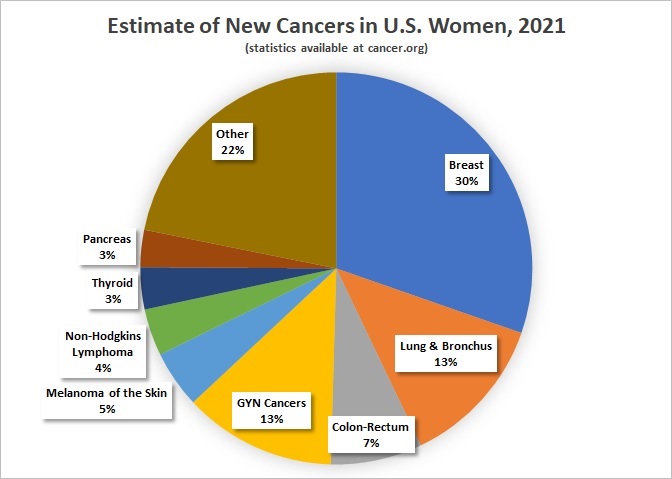
Which cancers are most likely to affect women?
Based on American Cancer Society Facts and Figures Excludes basal and squamous cell skin cancers and in situ cancers except urinary bladder cancer.
Breast cancer is the most common cancer in women. A woman’s lifetime risk of developing breast cancer is about 1 in 8. Breast, colorectal, lung, and gynecological cancers together represent over half of a woman’s cancer risk.
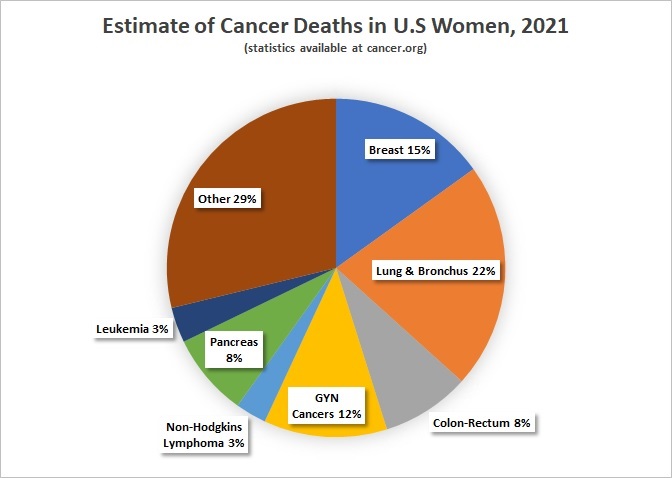
Which cancers are most likely to shorten a woman’s life?
Based on American Cancer Society Facts and Figures
In 1987, lung cancer surpassed breast cancer as the most frequent cause of women’s cancer deaths. The change reflects the fact that women’s smoking rates increased. The number of women who smoke peaked in 1965 at 34%, and daily cigarette consumption for women continued to rise into the 1980s.
Why are the statistics important to you regardless of your age?
These charts should impress you with how much of cancer is preventable. For many women’s cancers, prevention begins years before a woman is likely to develop the disease.
Lung Cancer: The National Cancer Institute states that 80% of women’s lung cancer deaths are due to smoking. Most women who smoke began before age 18. Women who smoke are 13 times more likely to develop lung cancer than those who have never smoked. (American Cancer Society Facts and Figures).
Breast Cancer: Breast cancer deaths have been declining steadily since 1990, thanks to better treatment and early detection (mammograms!). Still roughly 1/3 of women over 40 have not had a mammogram in the last two years. All women over 40 should have a mammogram every year! Women in higher risk groups may need to begin earlier or have additional studies as your physician recommends. Regardless of your age, you can take additional steps to reduce their lifetime breast cancer risk or increase the chances of finding a cancer at an early, more treatable stage.
- Know your family cancer history. Read more about family cancer syndromes.
- Make healthy choices. Breast cancer risk is 1.5 times higher in overweight women and 2 times higher in obese women. Newer research suggests that regular exercise can lower breast cancer risk as much as 10 to 20%, especially after menopause. Alcohol and tobacco use increase breast cancer risk. For alcohol, studies estimate a 7 to 12% risk increase for each serving a woman consumes on a daily basis. Longer periods of breastfeeding also seem to have a protective effect against breast cancer.
Gynecologic Cancers: These cancers develop in a woman’s reproductive organs, including the cervix, ovaries, uterus, fallopian tubes, vagina and vulva. Ovarian cancer is the most difficult to treat successfully, because it is difficult to find before it has spread beyond the ovary. The best preventive measures at any age include having annual well-woman check-ups. We can update your family cancer history and make recommendations for testing if needed. During your exam, we will inspect skin surfaces for signs of abnormal tissue.
Because of Pap tests, cervical cancer deaths have declined by more than half since 1975. We now know that a virus—human papilloma virus (HPV)—causes cervical and some other gynecologic cancers. The HPV vaccination has greatly reduced the risk of getting and spreading the virus. We recommend vaccination to our younger patients (before 27 years old) who missed the vaccine in their early teen years. We are also very pleased to help our patients who are moms of teens (boys and girls) understand the importance of HPV vaccination.
We also evaluate menstrual irregularities, especially bleeding between periods or after menopause. About 90% of women with endometrial cancer have irregular vaginal bleeding. Bleeding alerts us to the possibility of finding a cancer before it has advanced. Let your doctor know if you have bleeding, spotting, or an abnormal vaginal discharge. Family cancer history plays a role in some endometrial cancers (See Family Cancer Syndromes).
Colon and Rectal Cancer: Both new cases of colorectal; cancer and cancer deaths have been declining since the mid-1980s because of screening tests. Colorectal cancer is, to a large degree, preventable. The cancer screenings your doctor recommends save lives by finding colorectal cancers before they have spread and also by finding polyps (pre-cancerous growths) that may become cancerous. Other factors that influence your risk of colon cancer include your family cancer history (read about Lynch Syndrome) and certain lifestyle risk factors. Heavy alcohol use, obesity, and lack of physical activity are associated with a higher risk of colorectal cancer. Limiting your intake of red meat and increasing the fiber in your diet reduces your risk. The American Cancer Society reports that “for every 10 grams of daily fiber consumption there is a 10% reduction in colon cancer risk.”
So, to answer our question—are you old enough to worry about cancer? Worry doesn’t solve many problems. But awareness of preventive health strategies and lifestyle choices can make a real difference.